Subtotal $0.00
How glucose stability influences mood, cognition, stress, and emotional well-being
Blood sugar, also known as glucose, is often discussed in relation to diabetes. Yet its influence extends well beyond physical health. Glucose stability plays a meaningful role in concentration, emotional regulation, sleep, energy, and overall psychological well-being.
When blood sugar rises and falls sharply, the brain may interpret these shifts as physiological stress. For some people, this can appear as irritability, anxiety, fatigue, brain fog, low motivation, or mood changes. Emerging research increasingly points to a close relationship between metabolism and mental health, sometimes described as the metabolic and mental health connection.
1. How Blood Sugar Affects the Brain
The brain is highly dependent on glucose. Although it represents only a small proportion of total body weight, it uses a substantial share of the body’s available glucose to support memory, attention, decision making, and emotional regulation. When glucose supply is inconsistent, brain cells may struggle to maintain efficient communication.
- Low blood sugar, or hypoglycemia, may trigger the release of cortisol and adrenaline. These stress hormones can produce symptoms that resemble anxiety, including shakiness, sweating, racing thoughts, nervousness, and irritability.
- High blood sugar, or hyperglycemia, may contribute to inflammation, oxidative stress, vascular changes, and neurotransmitter disruption. Over time, these processes can affect mental clarity, energy, mood, and cognitive functioning.
- Frequent glucose spikes and crashes may also influence brain pathways involved in reward, motivation, serotonin, and dopamine. This may help explain why some individuals experience a temporary lift after sugary foods, followed by an emotional or energy crash.
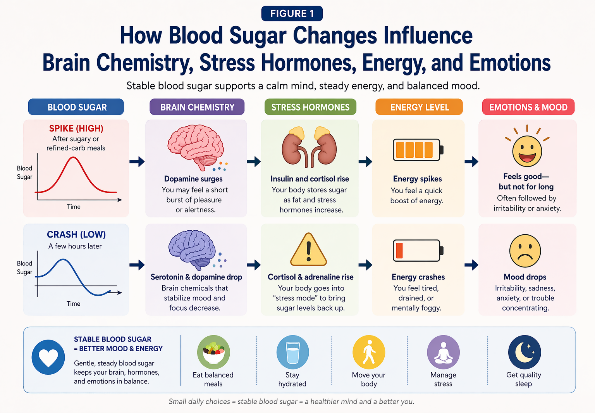
Figure 1. Infographic showing how blood sugar changes influence brain chemistry, stress hormones, energy, and emotions.
2. The Science Behind the Blood Sugar and Mood Connection
Blood sugar regulation and mental health influence each other in a two-way relationship. Stress, anxiety, poor sleep, and emotional distress can raise cortisol levels, which may increase glucose release into the bloodstream. In turn, persistently high or unstable glucose may intensify inflammation and oxidative stress, both of which are associated with depressive and anxiety symptoms.
This does not mean that every mental health concern is caused by blood sugar imbalance. Rather, it means that physical and psychological health are interconnected. A comprehensive approach to mental wellness should consider sleep, nutrition, stress physiology, movement, medical history, and emotional health together.
Research Highlights
| Condition or Pattern | Effect on Blood Sugar | Possible Mental Health Presentation | Example Source |
| Hypoglycemia | Drop in glucose with stress hormone activation | Anxiety-like symptoms, panic sensations, irritability | CDC, 2023 |
| Hyperglycemia | Inflammation, insulin resistance, and vascular stress | Depressive symptoms, fatigue, brain fog | Frontiers, 2024 |
| Glycemic variability | Sharp glucose spikes followed by crashes | Mood swings, tension, low energy | PMC, 2012 |
| High sugar intake | Impaired insulin response and metabolic strain | Increased risk of depressive symptoms | BMC Psychiatry, 2024 |
Clinical Interpretation
- People living with type 2 diabetes or prediabetes often experience higher rates of depression and anxiety than the general population.
- Inflammatory markers such as C-reactive protein and interleukin-6 may increase during metabolic dysregulation and may influence mood regulation.
- Even among individuals without diabetes, high-glycemic dietary patterns may contribute to fatigue, irritability, and reduced emotional steadiness.
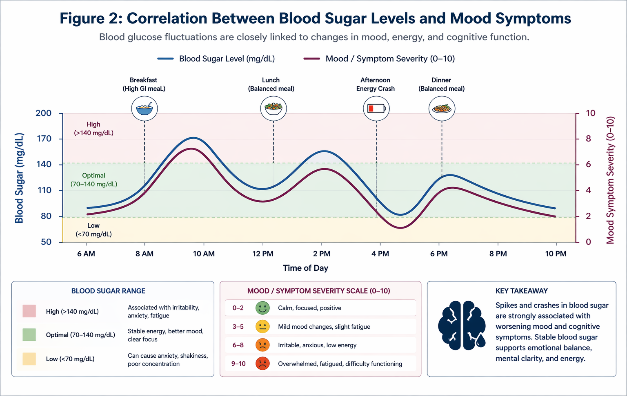
3. Symptoms That May Overlap With Mental Health Concerns
Blood sugar imbalance can mimic, worsen, or complicate mental health symptoms. This overlap can sometimes lead to incomplete treatment when the metabolic component is not explored.
- Fatigue and brain fog may occur when the brain does not receive a consistent glucose supply.
- Irritability or anger after meals may be linked to reactive hypoglycemia, especially after high-sugar meals.
- Anxiety, shakiness, or palpitations may occur when glucose dips, and adrenaline rises.
- Difficulty sleeping may be worsened by late-night glucose instability and disrupted hormonal rhythms.
- Low motivation or persistent sadness may be influenced by chronic inflammation, insulin resistance, and changes in dopamine signalling.
Recognizing these symptoms as possible metabolic signals does not replace psychological assessment. It simply broadens the lens and supports more integrated care.
4. Supporting Blood Sugar Balance for Better Mental Wellbeing
Small, consistent lifestyle changes can support both metabolic health and emotional stability. The goal is not perfection. The goal is steadier energy, clearer thinking, and a calmer nervous system.
Nutrition
- Eat balanced meals that include protein, healthy fats, and fibre to slow glucose absorption.
- Reduce refined carbohydrates such as sugary drinks, pastries, and white bread, which can create sharp glucose spikes and crashes.
- Choose lower-glycemic foods such as oats, beans, lentils, non-starchy vegetables, nuts, seeds, and berries.
- Avoid prolonged meal skipping if it worsens anxiety, irritability, or shakiness.
Movement
- Engage in regular physical activity, including walking, stretching, or light aerobic movement.
- Include strength-based exercises where appropriate, because muscle tissue helps the body use and store glucose more effectively.
Stress and Sleep
- Use stress-reduction practices such as deep breathing, prayer, mindfulness, journaling, or gentle movement.
- Prioritize sleep, because poor sleep can increase insulin resistance and intensify cravings.
- Stay well hydrated, as hydration supports circulation, concentration, and metabolic balance.
5. When to Seek Professional Support
Professional support is important when anxiety, low mood, brain fog, fatigue, sleep disturbance, excessive thirst, weight changes, or frequent shakiness persist. These symptoms may require both medical and psychological assessment.
Medical Support
- Ask a qualified health professional about blood sugar testing, including fasting glucose, HbA1c, or glucose tolerance testing where appropriate.
- Consider assessment of thyroid function, cortisol-related concerns, iron levels, and other medical factors when symptoms are persistent or unclear.
- Integrated care involving a physician, dietitian, endocrinologist, and mental health professional may be helpful when symptoms are complex.
Psychological Support
Seeking support from a qualified mental health professional can be an important step when stress, anxiety, low mood, or emotional eating patterns begin to affect daily functioning. Therapy can help individuals explore the emotional, behavioural, and physiological factors that may influence both mental well-being and blood sugar regulation.
Helpful coping strategies may include:
• Cognitive Behavioural Therapy: Supports individuals in identifying unhelpful thought patterns, managing stress responses, and building healthier routines.
• Mindfulness and self-compassion practices: Help calm the nervous system, reduce stress reactivity, and improve emotional regulation.
• Grounding and relaxation techniques: Deep breathing, body scans, prayer, journaling, and the 5-4-3-2-1 exercise can help reduce anxiety and restore calm.
• Lifestyle counselling: Helps translate health goals into realistic, culturally responsive, and sustainable daily habits.

Integrated care consultation focused on blood sugar, stress, and mood management.
Final Reflection
Mental health is not separate from the body. The brain, nervous system, hormones, immune system, and metabolism are in constant conversation. Blood sugar stability is one practical and often overlooked pathway through which people can support clearer thinking, steadier mood, and stronger emotional resilience.
For individuals experiencing persistent emotional distress, the most effective care is often integrative. Attending to nutrition, sleep, movement, stress, medical concerns, and therapy together can create a stronger foundation for healing.
Health note: This article is for educational purposes only and does not replace medical diagnosis or treatment. Individuals with diabetes, prediabetes, eating concerns, pregnancy-related health concerns, or persistent mental health symptoms should consult a qualified health professional.



